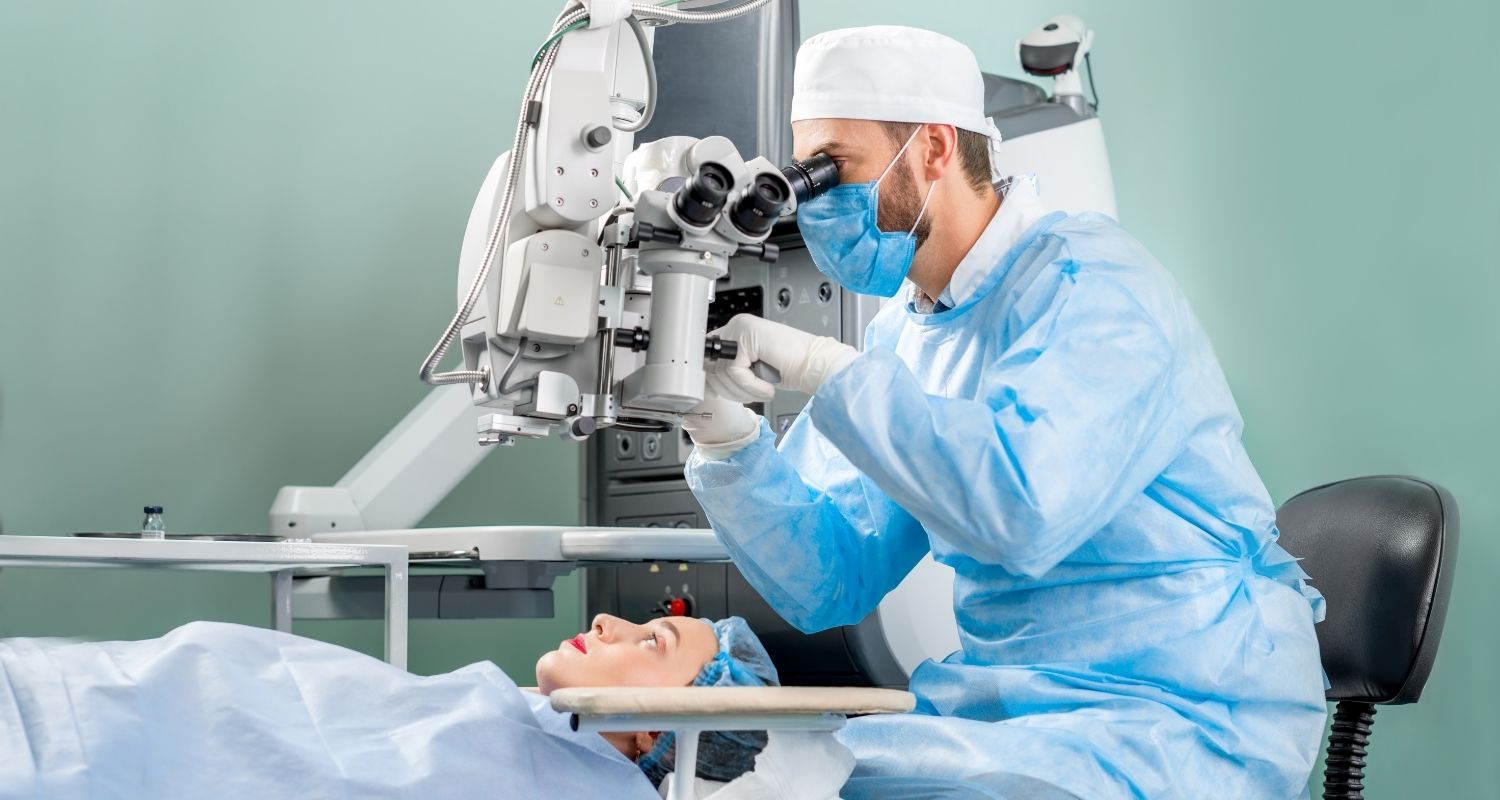
Cataracts occur when the natural lens in the eye becomes cloudy. This can cause gradual visual disturbance, affecting colour perception, night driving and quality of life.
Although it most commonly occurs after the age of 40, it can also be caused by a variety of factors. This includes infections, nutrition, eye trauma, smoking and diseases such as diabetes.
Commonly asked is how cataract surgery is carried out and will it last a lifetime? In this article, Gurjeet Jutley, Cataract Surgeon Oxford, explores the subject in more detail.
What is cataract surgery?
The nursing team assess each patient carefully, ensuring the full pupil dilation with drops. Within the operating room, the surgical team numb the eye before proceeding to make 2.4mm incisions that self-seal upon conclusion of the surgery. The cataract is ‘hoovered’ out before an acrylic lens is inserted to replace the previous one. Recovery usually takes 2-6 weeks and a protective eye shield is likely to be required at night.
If both eyes need treatment, surgery is usually undertaken weeks apart, although in some circumstances bilateral surgery may be considered. The new clear lens implants for cataracts are permanent and should last a lifetime. However, other condition affecting your eyes, such as diabetes or glaucoma, may mean limited vision irrespective of successful cataract surgery.
Risks and complications of cataract surgery
As with any other surgical procedure, risks of complications exist, varying depending on the eye and the type of cataract. Assuming that surgical complications are avoided, what is the natural lifespan and course of the lens. Well, approximately 20% of patients develop a posterior capsule opacification (PCO). This is a type of ‘scar tissue’ forming behind your lens implant. It’s caused when residual cells from the natural lens grow and migrate behind the lens and become sight impairing. Sight can often become blurred and cloudy, and you may experience issues with bright lights and glare.
Hence, affectively the impact of PCO can be fairly similar to the changes experienced when cataracts first came on, i.e. the ‘after-cataract’. Clearly, PCO can affect both eyes following bilateral surgery. This is not however absolute and the time gap between both eyes being affected may be large.
Certain factors may predict progression of PCO, such as: younger age at cataract surgery, inflammation and pre-existing ophthalmic conditions. However, it can occur in the setting of no other morbidities.
Fortunately, it is managed in an outpatient setting with treatment that is non-invasive and extremely effective.
Summary
The lens implant is inert and lasts a lifetime. Clouding of the capsule can occur in up to twenty percent of patients and is treatable in the outpatient setting.
Consultant Ophthalmologist, Gurjeet Jutley explains the treatment of posterior capsular opacification.